Pain in the back of the ankle or heel often involves the Achilles tendon. The following describes the tendon, common causes of pain and injury, how doctors evaluate problems, and treatment options from simple measures to surgery to help you discuss choices with your OrthoNJ care team.
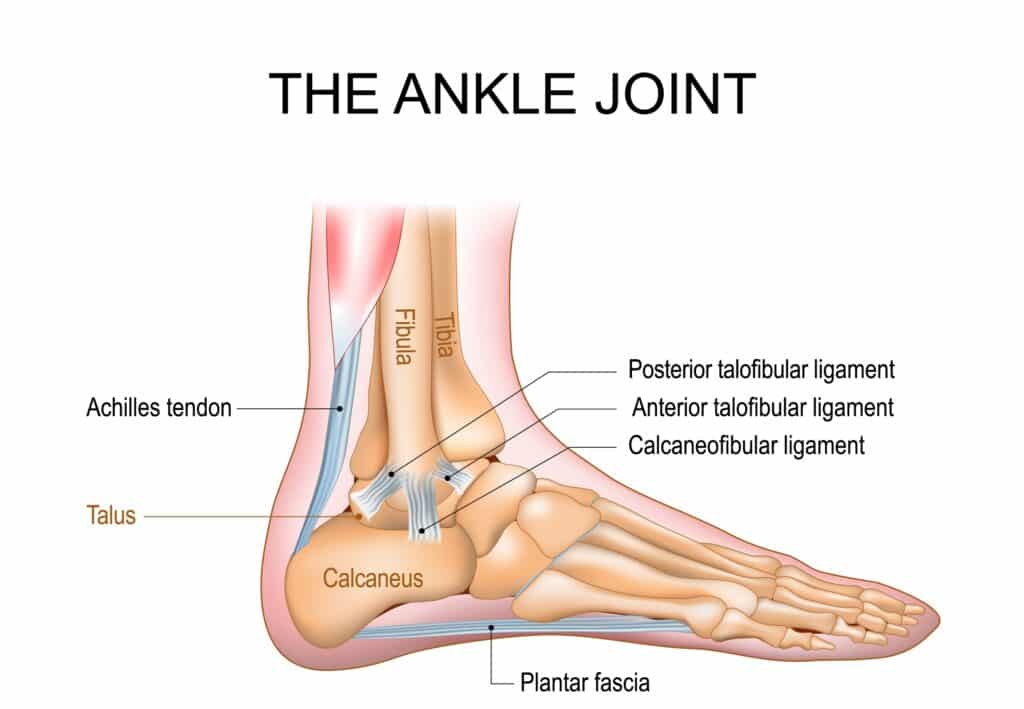
The Achilles tendon is the strong cord of tissue that connects your calf muscles to your heel bone. It helps you point your foot, rise up on your toes, walk, run, and jump.
Because it handles a lot of force during daily activities and sports, the Achilles tendon is one of the most commonly injured tendons in the body. Problems can range from short term irritation to a complete tear.
Most Achilles issues fall into two main groups:
Different parts of the Achilles tendon can be affected. Knowing the pattern helps guide treatment and expectations for healing.
Achilles tendinitis is irritation and inflammation of the tendon, often after a sudden increase in activity. Tendinosis refers to long term wear and degeneration of the tendon fibers without active inflammation.
These problems usually develop gradually and are more common in people who run, play jumping sports, or stand and walk a lot at work.
Doctors often describe Achilles issues based on where along the tendon the problem occurs.
| Type | Location | Typical Features |
|---|---|---|
| Noninsertional Achilles tendinopathy | Middle portion of the tendon, above where it attaches to the heel | Thickening of the tendon, pain with activity, often in younger and middle aged active people |
| Insertional Achilles tendinopathy | Where the tendon attaches to the back of the heel bone | Pain at the heel, possible bone spurs, more common in less active or older patients |
An Achilles tendon rupture is a partial or complete tear of the tendon, usually from a sudden strong push off or change in direction. It often affects active adults, especially men in their 30s to 50s who play sports occasionally.
Some ruptures happen in tendons that already have long standing wear and weakness, even if you did not have clear symptoms before the injury.
Symptoms vary depending on the type and severity of the problem. Not everyone has all the signs listed below.
With a sudden rupture, you might feel or hear a pop, followed by sharp pain and weakness. Many people describe feeling like they were kicked in the back of the leg.
Several factors can raise your chance of Achilles tendon problems. Some are related to activity, others to overall health.
Evaluation usually starts with a careful discussion of your symptoms, activities, and medical history, followed by a physical exam of your foot, ankle, and calf.
Imaging is sometimes used to confirm the diagnosis or to plan treatment:
Many Achilles tendon problems improve with nonsurgical care, especially when treated early. Your OrthoNJ provider will tailor a plan based on your diagnosis, activity level, and goals.
Reducing or pausing the activities that worsen your pain is usually the first step. This might mean cutting back on running, switching to low impact exercise like cycling or swimming, or taking breaks at work if you stand for long periods.
In some cases, a short period in a walking boot or heel lift may help decrease strain on the tendon while symptoms calm down.
Over the counter pain relievers such as acetaminophen or nonsteroidal anti inflammatory drugs (NSAIDs) may help ease pain and swelling. Not everyone can safely use these medicines, so follow your doctor’s guidance.
Ice packs placed over the back of the ankle for short periods can also provide temporary relief, especially after activity.
Steroid injections are generally avoided directly into the Achilles tendon because of an increased risk of tendon weakening and rupture. When corticosteroid injections are considered near the tendon, they are given cautiously and typically under specialist guidance with a careful discussion of risks and benefits.
Physical therapy is a key part of treatment for most Achilles tendon conditions. A therapist can guide you through stretches and strengthening exercises that gradually load the tendon in a safe way.
Your OrthoNJ provider or therapist will adjust the program based on your pain level and progress. It can take several weeks or months to see full benefits.
Supportive shoes with good cushioning and a slightly raised heel can reduce strain on the Achilles tendon. Avoid very flat or worn out shoes while you are recovering.
Some people benefit from custom or over the counter inserts that improve foot alignment and lessen stress on the tendon and heel. Heel lifts may also be used for a period of time under the guidance of your doctor.
Depending on your situation, your care team may discuss additional options such as specialized exercise programs, shock wave therapy, or other treatments that aim to stimulate healing in chronic tendon problems. The evidence and role of each option vary, so your doctor will review potential benefits and risks with you.
Surgery is usually reserved for people who still have significant pain or loss of function after a period of well guided nonsurgical care, or for certain tendon ruptures.
For long standing Achilles tendinopathy that has not improved with several months of treatment, surgery may involve removing damaged tissue, addressing bone spurs, and sometimes reinforcing the tendon with nearby tissue.
The exact procedure depends on whether the problem is in the middle of the tendon or where it inserts into the heel, as well as how much healthy tendon remains.
Both nonoperative and operative approaches are used for Achilles tendon ruptures. The best choice depends on your age, activity demands, other medical conditions, and how far the tendon ends have pulled apart.
Your OrthoNJ surgeon will discuss the pros and cons of each option, including differences in recovery time, risk of rerupture, and potential complications.
Rehabilitation is a major part of recovery for all Achilles tendon conditions, whether you have surgery or not. It focuses on restoring motion, strength, and confidence so you can return safely to your daily activities and sports.

Timelines vary by person and by treatment. Many people with tendinopathy notice steady improvement over several months. After a rupture, return to sports often takes many months, and sometimes longer than a year for high level activities.
Contact a healthcare professional promptly if you notice any of the following:
If you are unsure about your symptoms, OrthoNJ can evaluate your Achilles tendon, review your options, and help you choose a treatment plan that matches your needs and activities.
No treatment can guarantee a specific result or exact recovery timeline. Imaging findings and exam results must be considered along with your symptoms and goals. Some tendon changes reflect normal aging and may not need aggressive treatment. Many middle aged and older adults have imaging changes without significant symptoms, so treatment decisions are based on symptoms and function rather than imaging alone.
This information is meant for general education and is not a substitute for personal medical advice. Talk with your OrthoNJ provider about the approach that is safest and most reasonable for you.
If Achilles pain is limiting your work, exercise, or daily life, consider scheduling an exam with OrthoNJ. We will review your history, examine your leg and ankle, and recommend imaging or treatment options tailored to your situation.
Early, appropriate care often helps prevent problems from becoming long term and can support a safer return to the activities you enjoy.
Contact one of OrthoNJ's locations spread out through all of New Jersey.

This treatment info is for informational purposes only. Treatment and recovery vary person to person, and you should consult with your treating physician and team for details on your treatment and recovery process.