Lupus is an autoimmune disease that can affect your joints, skin, and many organs in your body. This guide explains what lupus is, common symptoms, ways it can affect your bones and joints, how doctors evaluate it, and main treatment options. It also describes how specialists at OrthoNJ can work with your rheumatology team to help manage joint pain and protect long-term mobility.
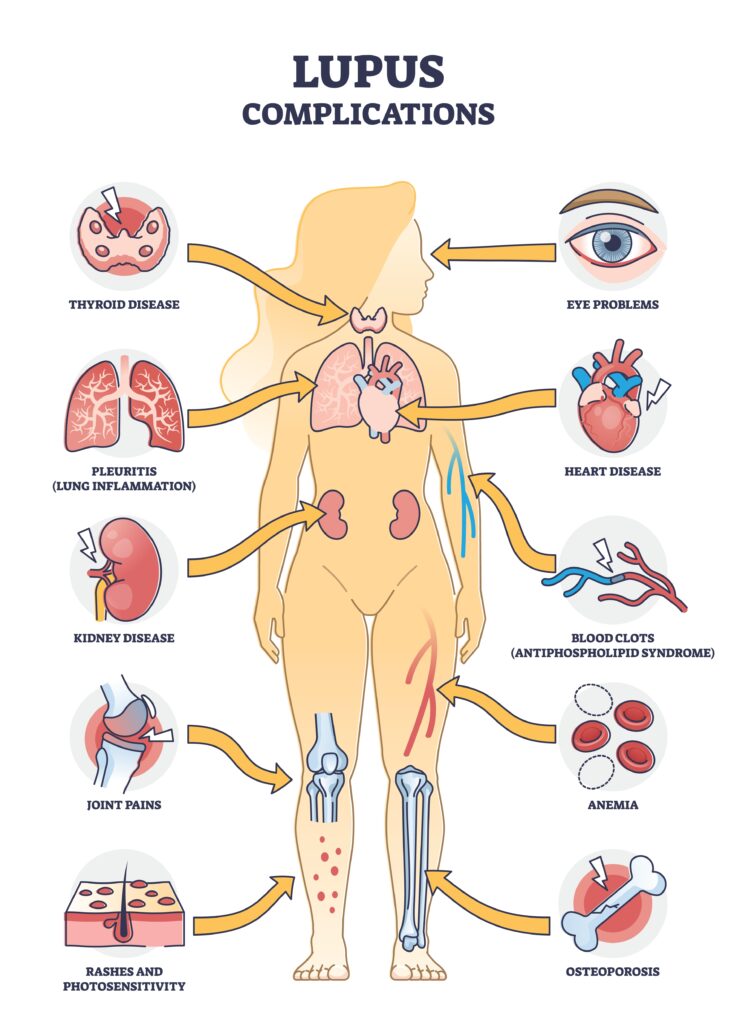
Lupus, also called systemic lupus erythematosus (SLE), is a chronic condition where the immune system mistakenly attacks healthy tissues. Inflammation can affect joints, skin, kidneys, lungs, heart, brain, and blood vessels. Symptoms often come and go in flares, with times of increased activity followed by periods of relative calm.
Although OrthoNJ specialists do not manage lupus as a whole, lupus can cause joint pain, bone loss, and tendon problems. OrthoNJ providers frequently work with rheumatologists and primary care doctors to address musculoskeletal effects such as arthritis, osteoporosis, and tendon injuries.
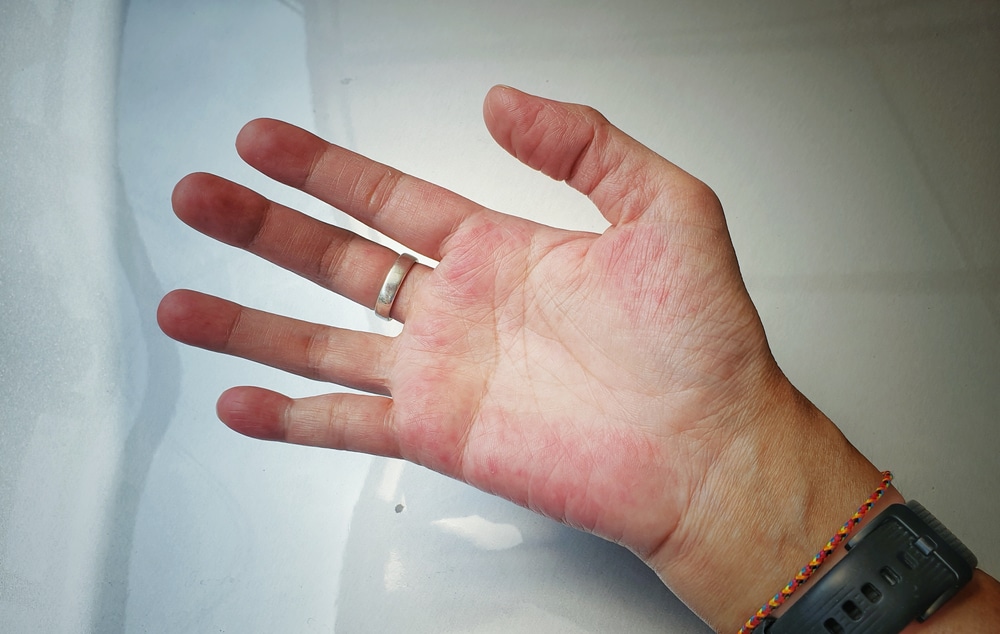
Lupus is an autoimmune disease. In a healthy immune system, the body recognizes and defends against infections. With lupus, the immune system becomes overactive and attacks healthy tissues, causing inflammation and tissue damage in different parts of the body.
The most common form is systemic lupus erythematosus (SLE), which can involve multiple organs. Other forms include cutaneous lupus, which mainly affects the skin, and drug-induced lupus, which is triggered by certain medicines and typically improves when the medicine is stopped.
Lupus can affect people of any age, sex, or ethnic background, but it is more common in women, especially those between ages 15 and 44. It occurs more often in people of African, Hispanic/Latino, Asian, and Native American descent than in white individuals.
Researchers think lupus arises from a combination of genetic risk, hormones, and environmental triggers such as certain infections, ultraviolet light, or some medications. A family history of autoimmune disease may increase risk, though most people with a family history never develop lupus.
There is no single test that proves lupus. Diagnosis is based on a combination of symptoms, physical examination findings, blood and urine tests, and sometimes imaging or biopsies. Many other conditions can look similar, so doctors will rule out other causes as part of the evaluation.
Rheumatologists usually lead the diagnostic process, especially when joint pain and autoimmune symptoms are present. OrthoNJ orthopaedic specialists may become involved if joint pain or structural damage is a major concern, and they typically work alongside rheumatology rather than replacing it.
Doctors may order tests to look for signs of inflammation and autoimmune activity and to see which organs might be involved.
Lupus symptoms vary from person to person and can change over time. Multiple body systems may be affected simultaneously.
Because lupus can mimic many other conditions, diagnosis can take time and careful evaluation. Tracking symptoms and bringing a written list to appointments helps your care team identify patterns.
Joint involvement is one of the most frequent problems in lupus. This is an area where OrthoNJ providers often join your care team, working in partnership with rheumatologists.
Orthopaedic care focuses on easing pain, maintaining function, and protecting bones and joints over time. Options may include bracing, activity guidance, physical therapy, and, in certain cases, surgery for severe joint or tendon damage.
Treatment aims to control inflammation, ease symptoms, protect organs, and improve quality of life. Because lupus presents differently in each person, treatment plans are individualized.
Rheumatologists usually direct medical treatment. OrthoNJ providers support this work by managing joint and bone problems, advising on safe activity, and treating specific orthopaedic issues when they arise.
Your rheumatology team will select medicines based on which organs are affected, how active the disease is, and your overall health. Not everyone needs the same medicines, and doses often change over time.
All these medicines have potential side effects, so regular follow-up and lab monitoring are important. Never change or stop lupus medications without consulting the doctor who manages your disease.
Daily habits can influence how you feel and how often flares occur. Lifestyle changes do not replace medication, but they often work together with treatment to help you stay active and independent.
Rheumatologists manage the overall disease process. OrthoNJ focuses on the musculoskeletal system to help preserve mobility and function when lupus affects joints, bones, muscles, or tendons.
Contact a healthcare professional promptly if you notice new or worsening symptoms that might suggest active lupus or complications.
In medical emergencies such as trouble breathing, chest pain, or signs of stroke, call emergency services right away. For joint-focused concerns like worsening pain or reduced mobility, OrthoNJ can assess your musculoskeletal health and coordinate with your rheumatology team.
Lupus is a long-term condition, and it is natural to have questions about the future. Many people live active lives with lupus when the disease is monitored and treated carefully. The pattern of disease is unique to each person, so treatment choices and activity recommendations should be tailored to you.
No single provider or test can guarantee a specific outcome. Imaging, lab results, and physical exams must be interpreted together. This article provides general education and is not a substitute for medical advice. Talk with your rheumatologist and, when joint or bone issues are a concern, with an OrthoNJ provider about the best plan for your situation.
If joint pain, stiffness, or mobility problems are affecting your daily life and you have lupus or suspect you might, consider scheduling an evaluation. Your rheumatologist can work with you on overall disease control, and OrthoNJ can help assess the impact on your joints, bones, and muscles.
Timely evaluation and coordinated care can help reduce pain, protect joint health, and support your ability to stay active long term.
Contact one of OrthoNJ's locations spread out through all of New Jersey.

This treatment info is for informational purposes only. Treatment and recovery vary person to person, and you should consult with your treating physician and team for details on your treatment and recovery process.