This article explains what cortisone shots are, how they work, when they may help, possible risks, how often you can get them, and what to expect before and after the injection. It’s written to help you talk with your OrthoNJ provider and make informed choices about your care.
Cortisone injections are a type of corticosteroid medication delivered directly into a painful joint, tendon area, or around a nerve. They are different from the steroids some people take for muscle building or hormone problems. Cortisone is designed to calm inflammation and can provide meaningful, though usually temporary, pain relief.
At OrthoNJ, we often use cortisone shots as one part of a broader treatment plan that may also include activity changes, physical therapy, oral medicines, and sometimes surgery. Not everyone is a good candidate, and the timing and location of injections matter. Your orthopedic specialist will help you decide if this option fits your situation.
Cortisone is a synthetic form of a hormone your body naturally makes in the adrenal glands. When used as an injection into a joint or the tissues around it, cortisone acts as a strong anti-inflammatory medicine. It doesn’t rebuild cartilage or reverse arthritis, but it often reduces swelling and irritation in the area.
By lowering inflammation, cortisone shots can ease pain, improve motion, and sometimes make physical therapy more comfortable and effective. Relief can last from several days to several months. The timing and degree of benefit are different for each person and for each condition.
Corticosteroid injections are commonly used throughout the body. Orthopedic specialists often recommend them for painful inflammatory problems in and around joints.
Not every painful joint benefits from a cortisone shot. Some types of pain are mainly mechanical, structural, or from nerve compression, and may respond better to different treatments. Your OrthoNJ provider will evaluate the source of your symptoms before recommending an injection.
Inflammation is your body’s response to injury or irritation. It can cause swelling, heat, stiffness, and pain. Cortisone interferes with the biochemical pathways that drive inflammation, which can lower those symptoms in the injected area.
When cortisone is injected into a joint or nearby tissues, only a small amount of medicine enters the bloodstream. Most of the effect is local. Some of the steroid is absorbed into the bloodstream and can cause short-term systemic effects, such as temporary increases in blood sugar or other effects in people with diabetes or certain other medical conditions. For that reason clinicians still need a full medical history before giving injections so they can weigh benefits and risks and plan any monitoring you may need.
Your orthopedic provider may suggest a cortisone shot if other noninvasive treatments haven’t given enough relief. It can also be used to calm a flare-up so you can better participate in physical therapy or daily activities.
In many cases, we start with options such as rest, activity changes, over-the-counter pain relief, and exercises. A cortisone shot becomes one more option if those steps aren’t enough or if symptoms are severe. In some situations, an injection also helps confirm the source of your pain by showing whether numbing and calming one specific area improves your symptoms.
Cortisone shots aren’t right for everyone. Some medical conditions or medications require extra planning or may make injections unsafe.
Always give your OrthoNJ clinician a full list of your health conditions and medications, including over-the-counter drugs and supplements, before scheduling a cortisone shot. This helps the team assess whether any short-term systemic effects are likely and how you should be monitored afterward.
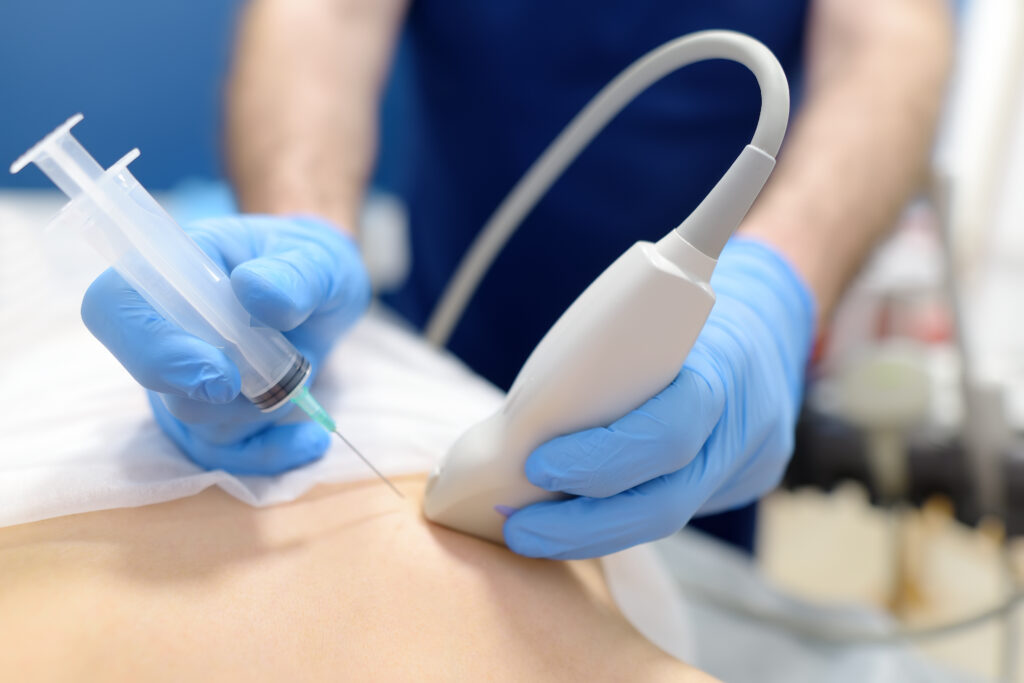
Cortisone injections are usually done in the office. For some deeper joints, such as the hip or spine, your doctor may use imaging guidance like ultrasound or fluoroscopy to place the needle in the most accurate position.
Most injections take only a few minutes once you’re positioned. You can typically go home shortly afterward and resume normal light activities the same day unless your provider gives you other instructions.
The numbing medicine, if used, often starts working within minutes and may give short-term relief for several hours. It’s common for pain to return for a day or two after that wears off. The steroid itself usually takes longer to have an effect, often several days and sometimes up to a week or more.
Some people feel clear improvement, some notice only mild change, and a few don’t respond at all. Relief may last from a few weeks to several months when it works well. Because responses are unpredictable, your provider can’t promise a specific level or duration of benefit.
Cortisone injections have been used for many years and are generally considered safe when used thoughtfully. Still, all medical procedures carry some risk. Your doctor weighs these risks against the potential benefits for your specific case.
Your OrthoNJ clinician will explain the specific risks that apply to the joint or area being treated, how often they occur, and what signs would require urgent follow-up.
There’s no single rule that fits every patient or every body part. In general, many orthopedic specialists limit cortisone injections in a specific joint to a few times per year. This approach aims to balance symptom relief with the possibility that repeated doses might affect cartilage, tendons, or other tissues.
As a general practice pattern many clinicians try not to exceed about three to four injections per year in the same joint depending on the diagnosis and the patient’s overall health because of concern about potential effects on cartilage or tendons. This is a typical guideline rather than a strict rule, and your provider will individualize the decision based on your health, how well prior injections worked, and other treatment options.
Corticosteroids can affect how the immune system responds and may influence healing. Because of that, many surgeons avoid giving cortisone injections in or near a joint too close to the time of certain operations, especially joint replacements.
Many surgeons avoid injections within a defined window often several weeks to a few months before and after some surgeries. The exact timing should be set by the operating surgeon based on current evidence and your individual situation, so be sure to discuss injection timing with the surgeon if you have upcoming or recent surgery.
Cortisone shots are usually just one tool in a larger treatment plan. They don’t cure arthritis or other chronic joint problems, but they can help you manage symptoms while you work on other strategies.
Right after the injection, many people can walk or use the arm as usual, but you may be advised to avoid heavy lifting, high-impact exercise, or repetitive strain for a short period. Your provider will give specific guidance based on the area treated.
Although serious problems after cortisone injections are uncommon, it’s important to know what signs need urgent attention.
If you’re unsure whether what you’re feeling is expected, contact your orthopedic office or another medical professional so they can advise you on the safest next steps.
Before deciding on a cortisone shot, it helps to have a clear conversation about your goals, other treatment options, and the potential benefits and limits of the injection. Bring a list of questions and your full medication and medical history to your visit.
At OrthoNJ, we’ll work with you to weigh cortisone injections against other approaches such as physical therapy, medications, activity changes, or surgery. The right plan is different for each person and often changes over time as your condition and activities change.
If joint or tendon pain is limiting your work, sleep, or activities, consider scheduling an evaluation with OrthoNJ. We’ll review your symptoms, perform a focused exam, and talk through options, which may include cortisone injections, therapy, medications, or other treatments tailored to your needs.
This information is meant for general education and shouldn’t replace a conversation with a qualified medical professional. Your OrthoNJ provider can help you decide whether a cortisone shot is appropriate for your specific condition and health history.
Contact one of OrthoNJ's locations spread out through all of New Jersey.

This treatment info is for informational purposes only. Treatment and recovery vary person to person, and you should consult with your treating physician and team for details on your treatment and recovery process.